Know Your Provider – Enrollment
KYP Enrollment provides an electronic solution to review applications of all newly enrolling, re-enrolling, and revalidating Medicaid providers. It ensures that these providers meet participation eligibility requirements prior to enrolling or continuing enrollment in the program as mandated by ACA Part 455 Subpart E requirements.
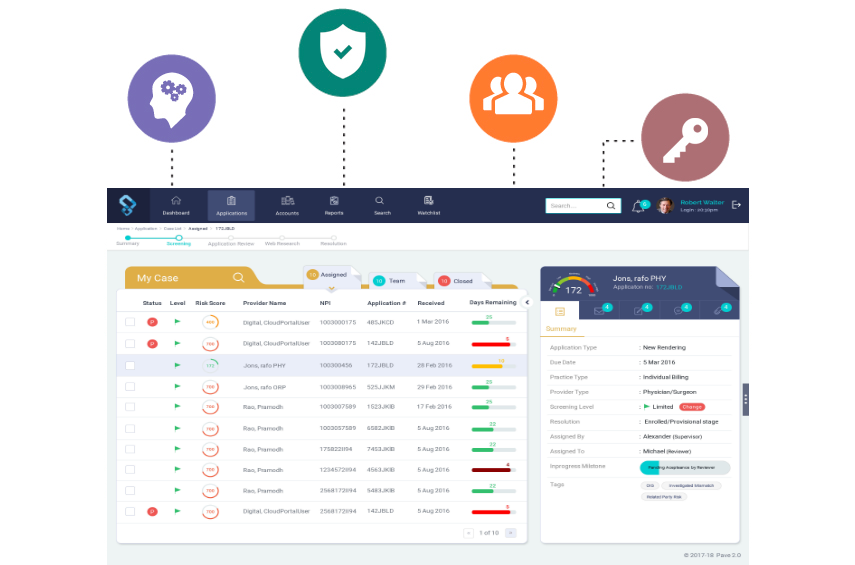
A Paradigm Shift In
Provider Enrollment Application Services
- Gives complete control on managing provider applications
- Increases efficiency of users through digitization and automation
- Reduces process cycle times and enhances adherence to SLAs
- Improves customer service through superior interaction and collaboration
Key Capabilities
- Centralized Application List Centrally manages electronic as well as paper-based applications
- Account Lifecycle Automates account opening after successful enrollment and provides subsequent management
- Document and Form Review Supports electronic review of provider form and documents
- Communication and Collaboration Letter generation, messages to internal users and providers and ability to consult peers
- Configurable Workflow Automates workflows for new provider, supplemental updates, change of ownership, address and more
- End-to-end ‘Smart’ Solution Integrates with KYP Portal and Screening for complete provider lifecycle management
